Newsletter 2020
Newsletter October 2020: Application of a device in times of pandemic: Safety for the patient and medical personnel
Niño MC, Pauwels A, Raffan F, Arango E, López JP.
Introduction
In Colombia, 500,000 COVID-19 cases and 15,800 deaths have been reported, among which health personnel cases and deaths amount to 5,619, and 43 respectively (1). Age is an independent risk factor for suffering from a severe disease, with the ages of 65 and over representing the highest risk. In the US, individuals over the age of 65 represent 45% of hospital admissions, 53% of intensive care unit admissions, and 80% of fatalities (2). In Colombia, the installed capacity of beds in the ICU for the care of COVID-19 increased by 36%, most of them in mechanical ventilation. The increase in life expectancy and the decrease in the birth rate have led to a significant increase in the average age of the population, where probably a third of geriatric patients will undergo a surgical procedure (3). From the anaesthetic point of view, this has implications in airway management due to an increase in the difficulty of positive pressure ventilation.
On the other hand, the highest viral load of SARS-CoV-2 has been reported in sputum and secretions of the upper respiratory tract, especially nasal (4). However, tracheal intubation is considered a high-risk procedure for health personnel due to the risk of exposure by aerosolisation (5). For this reason, in airway management, the most experienced professional should be chosen, simulation exercises of personal protective equipment protocols implemented, adequate spaces to manage the airway allocated, airway management equipment for patients diagnosed with or suspected of having COVID-19 made available, necessary or potentially necessary medications guaranteed, airway management guidelines in times of pandemic developed further, and the situations that lead to potential aerosolisation avoided or reduced.
Device description
In 2017, the authors first published the description of a new device for the ventilation of edentulous patients called NIPARA, (NI) Niño, (PA) Pauwels, (R) Raffan, and (A) Arango, demonstrating a significant improvement in the coupling of the face mask by an increase in positive pressure ventilation and a decrease in the loss of escape volume between the mask and the patient, which in theory reduces the potential aerosolisation of this intervention.
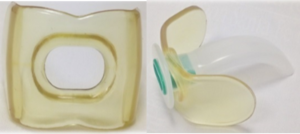
The device consists of an intraoral extended U-shaped plastic plate, latex-free plastic materials (4.6 inches x 1.4 inches) with right and left side extensions. In the midline, it has a mating surface on both the top and bottom that engages the labial frenulum allowing intraoral retention, and the lateral extensions are placed between the gums and cheeks. The device is inserted using the same insertion technique as conventional oropharyngeal cannulas inserted into the device’s central hole. Once the NIPARA is inserted, the face mask is used as usual by resting it on the patient’s face for manual positive pressure ventilation before the intubation of the patient. –Figure 1. (6).
Discussion
Ventilation with a face mask is a procedure that produces a high degree of aerosolisation, and all the strategies that decrease it, such as two-hand ventilation and two operators providing an adequate seal to the face or rapid sequence induction, are indicated in the time of induction of anaesthesia. Assessment of the airway’s difficulty in COVID-19 patients can be carried out with the MACOCHA scale before the procedures (7).
This article mainly focuses on the face mask ventilation manoeuvre in the emergency, resuscitation, surgery, or intensive care setting, where patient and staff protection is essential. Therefore, according to the principles of the Safe Airway Society for the management of the airways and endotracheal intubation for the group of adult patients with COVID-19, it is crucial to follow the rapid sequence intubation protocol, to decrease long periods of high-flow oxygenation or non-invasive ventilation because of its potential aerosol generation. Due to the proximity of the medical staff to the patient’s airway, it is essential to minimise the risk of aerosolisation generation with these procedures (8). Among the predictors of difficult ventilation are edentulous patients, since it is difficult to obtain an adequate seal between the mask and the patient’s face due to the loss of vertical dimension, allowing air leakage (9).
In the first semester of 2020, during the COVID-19 pandemic, 4,951 patients have been operated on at Fundación Santa Fe de Bogotá University Hospital, Bogotá, Colombia.
Around 27% (a group of 1,347 patients) were over 60 years of age, for which the possibility of being edentulous according to the National Study of Oral Health of Colombia is approximately 33%, which is probably equivalent to 440 patients that required some support of the airway and surely to be ventilated with the safety protocols. Thus, by restoring the vertical facial dimension of edentulous patients with NIPARA, a better adaptation of the facial mask is achieved and lower resistance to ventilation, thus reducing the possibility of particle aerosolisation (10).
Conclusion
This article does not intend to change the safety protocols already established or indicate mask ventilation in all patients. However, if necessary, the NIPARA can be a low-cost device, a useful, easy-to-use, and safe tool taking into account that the population older than 65 represents a high percentage of patients who go to hospitals and require ventilation either in endoscopy procedures, surgery, intensive care unit or in an emergency room. Additionally, they present total edentulism, making it difficult to seal between the marking and the patient’s face, generating an aerosol outlet with a high risk of contamination.
Figure 1. NIPARA device.
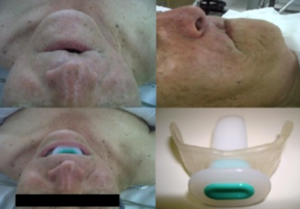
Figure 2. A patient using and not using NIPARA before ventilation
References
- Ruiz-Gómez F. https://covid19.minsalud.gov.co/
- Antunes B, Bowers B, Winterburn I, et al. BMJ Support Palliat Care. 2020; 10: 343.
- Nazar C, Zamora M, Fuentes, Lema G?. Rev Chil Cir, 2015; 67: 309.
- Wang W, Xu Y, Gao R, Lu R, Han K, Wu G, Tan W. JAMA, 2020; 323: 1843.
- Wu Z, McGoogan JM.. JAMA. 2020;v323: 1239.
- Niño MC, Pauwels A, Raffan F, Arango E, Romero DJ, Benitez D.. Expert Rev Med Devices, 2017; 14: 315.
- Atherton F, Calderwood C, McBride M, Whitty C, Powis P, Melville C Supporting doctors in the event of a Covid-19 epidemic in the UK. General Medical Council. 2020.
- Brewster DJ, Chrimes N, Do TB, Fraser K, Groombridge CJ, Higgs A, Humar MJ, Leeuwenburg TJ, McGloughlin S, Newman FG, Nickson CP, Rehak A, Vokes D, Gatward JJ. Consensus statement: Safe Airway Society principles of airway management and tracheal intubation specific to the COVID-19 adult patient group. Med J Aust. 2020; 212:472.
- Racine SX, Solis A, Hamou NA, Letoumelin P, Hepner DL, Beloucif S, Baillard C. Face mask ventilation in edentulous patients: a comparison of mandibular groove and lower lip placement. Anesthesiology. 2010;112:1190.
- Peñaloza RE, Palacio Y, Gómez LC, Becerra AM, Amaya JL, Suárez E. Estudio Nacional de Salud Bucal IV, Ministerio de Salud y Protección Social 2013-2014.
More Newsletter Articles
Visit our Euroanaesthesia 2020 Website for more news on everything related to the virtual congress.
Visit our COVID-19 Resource Hub for other news and resources.