Newsletter 2022
Newsletter April 2022: News from Ukraine
Experience in the treatment of the wounded patients, hospitalised in the Kyiv trauma centre in the first days of the war in Ukraine
Sergii Dubrov, Stepan Cherniaiev, Maksym Denysiuk, Sergii Sereda, Yurii Zaikin, Lianskorunskyi Volodymyr
National Medical University named after O.O. Bogomolets
sergii.dubrov@gmail.com
At 0500H on February 24, the whole of Ukraine woke up to the sounds of explosions. Russia launched a war against Ukraine without warning, and Russian troops began bombing civilian and military infrastructure, primarily airports. From the first hours of the war, dozens of people with gunshot, blast injuries and burns were hospitalised in our clinic.
We, the authors of this article, work in the municipal hospital, which is the multiple trauma centers in Kyiv, where the vast majority of victims were hospitalised. In this case, the experience of the hospital staff that was received in February 2014 during the “Revolution of Dignity” in Kyiv, when 157 patients with multiple gunshot wounds were hospitalised in 2 days in our institution, was very useful. It allowed medical personnel to provide high-level sorting of patients during multiple admissions.
Within hours of the bombing, most of the doctors and nurses arrived at the hospital. At the beginning of the war, the hospital was fully equipped with blood products (red cell mass, fresh frozen plasma); infusion solutions; antibacterial and analgesic drugs, as well as all consumables and equipment to provide the necessary medical care to the victims in the required amount.
We have 28 ventilators for 16 beds in the ICU and 5 operating tables, which allowed us to perform surgical interventions and primary surgical treatment not only in the operating room but also on wheelchairs and beds in the ICU. Medical registration of the wounded patients was performed in the admitting area during the multiple admissions, at the same time E-FAST protocol was carried out, after which the patient was sent to the observation ward or an additional X-ray or CT was performed, depending on the severity of the patient’s condition.
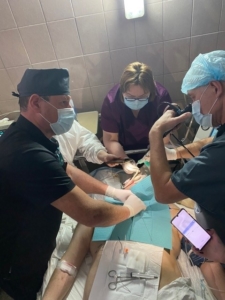
After the massive shelling of civilian infrastructure, up to 6-7 patients were required to perform simultaneous interventions, involving 5 to 9 health workers per patient, and in some cases two teams of surgeons (neurosurgeons and abdominal/thoracic surgeons or traumatologists). To stabilise the vital functions and ensure anaesthesia of extremely severe patients, we had the opportunity to involve 2 anesthesiologists and 2 nurse anaesthetists at the same time.
Analysing the intermediate results of our work for the first 10 days since the beginning of the war (from February 24 to March 3, 2022) medical care in the clinic was provided to 203 patients, of whom 84 (41.4%) were outpatients, which included general examination of the patient; performing routine laboratory tests; X-ray and ultrasound examinations or CT scans, if necessary, minor surgical interventions, such as primary wound management was performed.
Among all patients who were transported to the hospital, 119 (58.6%) of all patients required hospitalisation, of them the vast majority – 89 (74.8%) patients received injuries related to hostilities (gunshot, blast injuries and burns), and 30 (25.2%) patients had traumatic injuries not directly related to hostilities (road accidents; falls from a height; domestic violence). In total, for the period from February 24 to March 3, 2022, in our trauma centre, 119 patients underwent 172 surgeries.
In this review, we would like to focus directly on the analysis, structure of injuries and surgical interventions in 89 hospitalised civilian patients who received injuries as a result of hostilities, for the period from February 24 to March 3, 2022.
Despite the fact that our hospital specialises in providing care to adult patients with traumatic injuries, under these extraordinary conditions, 4 children were hospitalised in our clinic. The age of patients ranged from 13 to 86 years (38.61 ± 15.53 years). According to the gender distribution, there were 11 women (12.4%) and 78 men (87.6%). The number of patients with lesions of one anatomical area was 54 (60.7%), with lesions of two or more anatomical areas – 35 (39.3%). 61 (68.5%) injured patients required from 2 to 6 surgical interventions, which was due to damage of various anatomical areas or the need for phased surgery, including the use of the damage control strategies. Combined mine blast/gunshot and burn injuries occurred in 4 (4.5%) patients, 2 (2.2%) patients were hospitalised with traumatic injuries and hypothermia, and 8 (9.0%) patients with stab wounds. Table 1 shows an anatomically based structure of mine blast and gunshot injuries in hospitalised patients.
Anatomically based structure of mine blast and gunshot wounds in hospitalized patients
|
Anatomical area |
Number of patients | Penetrating | Not penetrating |
| Head and neck | 27 | 20 | 7 |
| Face | 8 | 6 | 2 |
| Chest | 31 | 23 | 8 |
| Abdomen or pelvic contents | 19 | 14 | 5 |
| Extremities or pelvic girdle | 66 | – | 66 |
| Total | 151 |
63 |
88 |
Table 1
In order to prevent and treat hypothermia, almost all patients in the operating room were warmed by using a patient warming system and thermal blankets, infusion solutions used during surgery were warmed to 36°C in a thermostat.
During the multiple admissions of extremely severe victims, surgical interventions were carried out on the principle of a damage control strategy, which consisted of surgical haemostasis, emergency interventions of moderate/reduced surgery, further stabilisation of vital functions and correction of coagulopathy and electrolyte imbalance in the intensive care unit, then the required extent of full surgery in the delayed period was performed, within 24-72 hours.
Of the 66 patients with extremities or pelvic girdle injuries, mine explosions or gunshot fractures of the long limb bones were detected in 41 injured patients and all were treated according to the damage-cоntrol orthopaedic strategy. Immediately after hospitalisation, they underwent fracture stabilisation with external fixation devices, followed by vacuum-assisted closure therapy for open skin and soft tissue injuries, after which the final internal osteosynthesis was performed.
Damage-control surgery for abdominal injuries strategy was used in 5 cases, among which were massive liver damage (3 patients), and multiple intestinal injuries (2 patients). In two patients, the damage-control surgery strategy was used for injuries to the pleural cavity.
In total, out of 89 patients hospitalised with traumatic injuries received as a result of hostilities, 9 (10.1%) died. Among the dead, almost half of the wounded were hospitalised in a clinical death – 4 (44.4%) patients. Two patients (22.2%) died in the operating room within the first hours of hospitalization, two more patients died within the first day after injuries and one victim had a penetrating skull and gunshot wounds to the abdominal organs (liver and intestines) died from complications in the delayed period.
Considering the implementation of curfew, significant restrictions on travel in the city by car, disruption of public transport, the lack of fuel at gas stations, part of the personnel were unable to get to the hospital or home, as a result, about half of all hospital staff since the first day of the war have not yet left the hospital. A large proportion of hospital staff, including the authors of this publication, consider it their duty to make every effort to save the lives of the patients, which is why they (we) have been living in the hospital since February 24.
The problems we faced in the first days of the war were related to the logistics of providing food for patients and medical staff, as the hospital catering became unavailable on February 25, as well as food delivery for staff. On the morning of Saturday, February 26, reserves of drinking water and food were depleted, but thanks to the efforts of volunteers, by noon the same day, despite the constant shelling, an uninterrupted supply of food and water was established.
Indeed, a great role in providing quality medical care and solving household problems belongs to volunteers who offered their help, the amount of which far exceeded our needs. Volunteers were involved in cooking, cleaning, washing dishes, and washing clothes, as centralised services were unavailable due to the warfare. A special mention should be made to the contribution to the delivery of health care by medical students who acted as nursing staff in the hospital, assisting more experienced nurses.
We would also like to thank the organisations and individuals in Ukraine, the European Union, the United Kingdom, the United States and other countries that provided humanitarian assistance in the form of medical equipment, drugs and consumables for healthcare facilities in Ukraine.
Also, our thanks are directed towards the governments, doctors and people from countries of the world for the assistance and financial and moral support, which is extremely important for every Ukrainian. We would like to single out the contribution of numerous professional medical organisations, in particular ESAIC which provided an opportunity for Ukrainian doctors to join educational resources and training free of charge!
[maxbutton id=”1″ url=”https://www.esaic.org/newsletter/” text=”Read the Newsletter” ]